Patient care doesn’t happen in a silo—in any given hospital stay, a patient could have a dozen different clinical and operational staff contributing to their care. Even beyond ancillary departments like radiology and labs, operational departments such as housekeeping, nutrition and pharmacy can all collaborate with clinical staff to build the care plan or otherwise interact with the patient. When there are so many variables and influences on the patient, healthcare organizations can’t afford to overlook cross-departmental collaboration.
The Impact of Enhanced Collaboration
Every healthcare organization is different—oftentimes workflows will even vary facility to facility and unit to unit. However, one thing we see across nearly every hospital is cross-team collaboration. A nurse collaborates with other nurses, yes, but he also collaborates with hospitalists, specialists and support staff. A communication tool that only allows him to communicate with other nurses limits the scope of his reach. This is why, when we speak with healthcare leaders about communication and collaboration tools, we usually suggest onboarding all users across the care environment to maximize value and workflow productivity.
Expanding the reach of users throughout the healthcare continuum can have a significant impact on patient outcomes. Over thousands of interactions in a single shift, we’ve seen quicker communication and collaboration expedite the entire workflow.
For instance, instantaneous communication between the patient’s care team and the radiology department can improve turnaround time by 20 percent. The emergency department can shorten door-to-balloon time by 15 percent when they can easily reach specialists and bed coordinators in other departments with the tap of a button.
Finally, when clinicians spend less time running around looking for their colleagues, they can spend more time at the patient bedside. Our customers have seen a 7 percent increase in patient satisfaction scores after implementing MH-CURE in this way.
The Value of Multidisciplinary Care
After hundreds of go-lives in healthcare organizations across the country, we’ve gathered average communication data that demonstrates the communication pathways clinical and operational staff use every day.
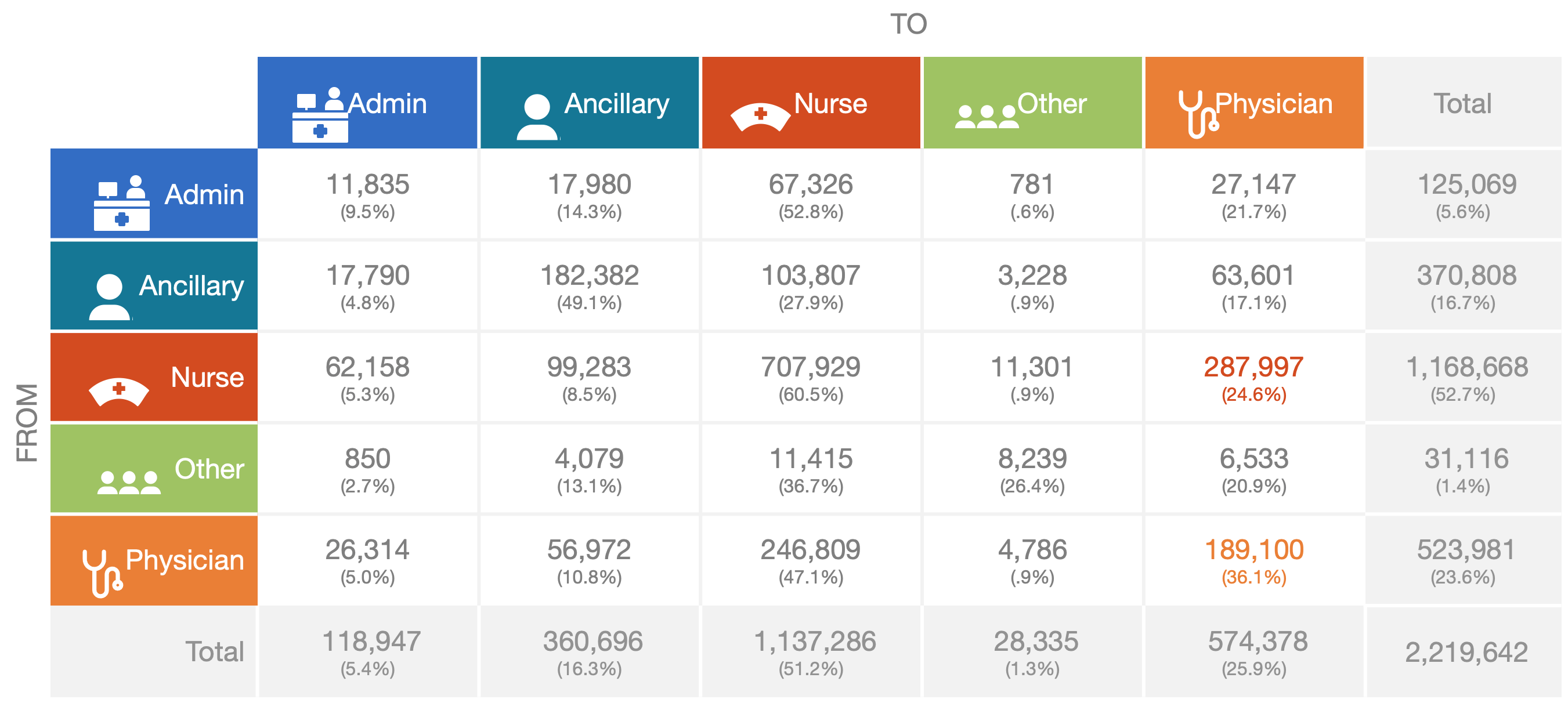
Notably, nurses and providers use communication tools to reach more than just other nurses and providers. While nurse-to-nurse and physician-to-physician communication events are frequent, these clinicians still initiate and receive calls, texts and more from ancillary staff. There’s a name for this phenomenon: Metcalfe’s Law. It states that the value of a communication network increases exponentially with each additional user added.
In fact, collaborative tools that support multidisciplinary care can not only improve common care coordination workflows, they can also mitigate symptoms of clinical burnout caused by communication challenges. Research has shown organizational changes to the hospital environment—such as improving and expediting user access to colleagues—can alleviate clinicians’ cognitive burden by reducing the number of times they need to switch between devices and applications to advance care.
Supporting multidisciplinary collaboration has always been one of the pillars of our software applications. We have a decade’s experience working with healthcare employees from countless departments to enhance and optimize workflows for quicker time to care; we’ll continue to use this expertise to support and enable clinicians to advance care.
To learn how we can improve outcomes at your organization, schedule a consultation with our clinical mobility team.